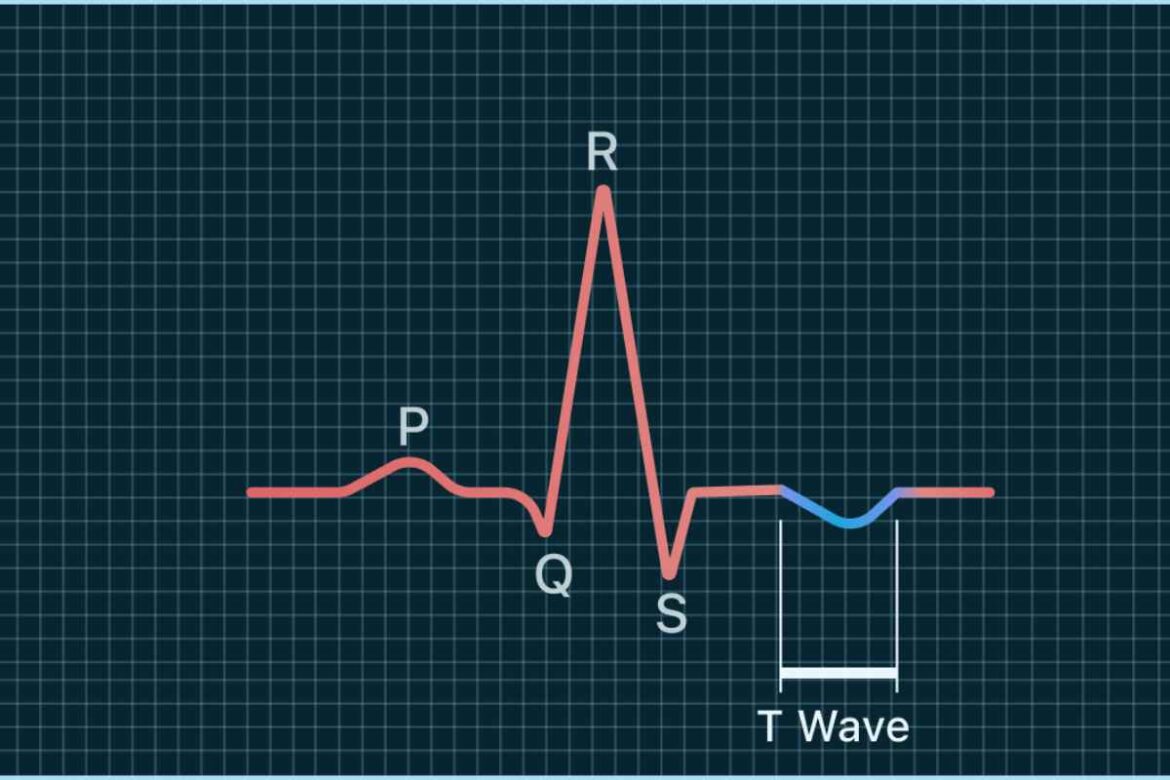
Seeing “abnormal T wave” on a test result can be unsettling. Most people do not know what that phrase means, and the internet can make it sound worse than it is. A calmer place to start is this: a T wave is one part of an ECG, the heart tracing that shows electrical activity, and a change in that pattern does not always point to one clear diagnosis.
Sometimes there are no noticeable symptoms at all. In other cases, symptoms happen because of the issue behind the ECG finding, not because the T wave itself can be felt. That is one reason abnormal t wave symptoms can be confusing. The tracing may reflect something temporary, something benign, or something that needs a closer look.
What an abnormal T wave can mean
The T wave represents the heart’s recovery phase after each beat. On an ECG, clinicians look at its shape, direction, and timing. Research shows that T-wave changes can appear in a range of situations, including electrolyte shifts, medication effects, strain on the heart, inherited rhythm conditions, and structural heart disease. In some people, certain T-wave patterns can also be seen without serious disease, especially depending on age, training status, and the full ECG context.
That context matters a lot. A single abnormal-looking T wave does not tell the whole story. Clinicians usually interpret it alongside symptoms, medical history, medications, family history, blood work, and other parts of the ECG.
Can an abnormal T wave cause symptoms by itself?
Usually, people do not “feel” a T-wave change directly. What they may feel are symptoms related to the reason the ECG looks different.
That distinction helps. It means a person can have a T-wave abnormality and feel completely normal, or feel quite unwell for reasons that are only partly reflected on the ECG.
Common symptoms that may show up with an underlying heart or rhythm issue include:
- palpitations, or a sense that the heart is fluttering, racing, or skipping
- dizziness or lightheadedness
- fainting or near-fainting
- chest discomfort
- shortness of breath
- unusual fatigue
- exercise intolerance, meaning activity feels harder than usual
These symptoms are not specific to one condition. They can happen with heart-related problems, but they can also occur with anxiety, dehydration, stimulant use, medication effects, or other noncardiac causes. That is why interpretation should be done by a qualified clinician rather than by pattern-matching online.
When there are no symptoms
Many T-wave changes are found incidentally, which means they show up during a routine ECG, a pre-op test, a sports screening, or an evaluation for something unrelated.
In that situation, the next question is usually not “What symptoms should I expect?” but “What does this finding mean in my case?” The answer depends on the full picture. Some ECG changes are temporary. Some reflect normal variation. Some deserve follow-up because they may be linked with conditions that affect heart rhythm or heart muscle function.
A person without symptoms may still be advised to have repeat testing, medication review, lab work, or a cardiology visit. That is not always a sign of danger. Often, it is just careful medicine.
Why T waves can look abnormal
There is no single cause. T-wave morphology, meaning the shape and appearance of the T wave, can change for several reasons.
Possible contributors include:
- electrolyte imbalances, especially potassium-related changes
- certain medications that affect the heart’s electrical system
- reduced blood flow to the heart
- inflammation or strain involving the heart
- inherited rhythm conditions such as long QT syndrome
- structural heart conditions, including some cardiomyopathies
- changes seen after altered conduction patterns or procedures
- normal variants in some healthy people
Research on T-wave morphology has also shown that some patterns may help specialists identify higher-risk rhythm conditions, but those findings are nuanced and not something most people can interpret from a printed ECG alone. Even among experts, meaning depends on the exact pattern and the clinical setting.
When it may matter more
Some situations deserve more attention than others.
T-wave changes may carry more weight when they appear along with fainting, strong palpitations, chest pain, unexplained shortness of breath, or a personal or family history of arrhythmia, sudden cardiac death, or inherited heart disease. They may also matter more when they are new, widespread across several ECG leads, or paired with other ECG abnormalities.
Another important point is persistence. A one-time tracing can be useful, but repeat ECGs sometimes show that a change was temporary. In other cases, a repeated pattern supports the need for further evaluation.
To keep this grounded: the ECG is a clue, not a final conclusion.
How doctors usually evaluate it
Evaluation often starts with simple questions:
- What symptoms are happening, if any?
- Did they start suddenly or change over time?
- Are there any new medications or supplements?
- Is there a family history of fainting, arrhythmia, or sudden death?
- Are there other health issues, such as high blood pressure or known heart disease?
From there, a clinician may recommend repeat ECG testing, blood tests, a heart monitor, an echocardiogram, or referral to a cardiologist. The goal is to understand whether the T-wave pattern is a normal variation, a temporary change, or part of a condition that needs treatment or monitoring.
When it comes to logistics, it can help to bring a medication list, any prior ECGs, and a short note about symptoms and when they happen. That often makes the visit more useful.
Anxiety can complicate the picture
Heart-related symptoms and anxiety symptoms can overlap more than people expect. Palpitations, chest tightness, shortness of breath, and dizziness can happen in both settings. That overlap can leave people feeling embarrassed, uncertain, or afraid they are missing something serious.
A careful clinician should not dismiss symptoms as “just anxiety” without considering the full picture. At the same time, anxiety can absolutely intensify body awareness and make normal sensations feel alarming. Both things can be true: the symptoms feel real, and the explanation may still be less dangerous than you fear.
A realistic way to think about it
An abnormal T wave is not a diagnosis. It is a sign on a tracing that needs interpretation in context.
For many people, the outcome is reassurance after a more complete review. For others, it leads to follow-up that helps catch a rhythm issue, medication effect, electrolyte problem, or heart condition that needs attention. Neither response is overreacting. It is simply the reason ECGs are interpreted as part of a bigger clinical picture.
Conclusion
This kind of result can stir up a lot of worry, especially when the wording sounds technical and final. In reality, T-wave changes can mean different things, and symptoms do not always line up neatly with what appears on an ECG. The most useful next step is not guessing from the report alone, but having the finding interpreted with your symptoms, history, and any other test results in view.
If you have been told your ECG showed this change and you are unsure what it means, a medical follow-up can give you a clearer answer than the result line by itself.
Safety Disclaimer
If you or someone you love is in crisis, call 911 or go to the nearest emergency room. You can also call or text 988, or chat via 988lifeline.org to reach the Suicide & Crisis Lifeline. Support is free, confidential, and available 24/7.
Author Bio
Earl Wagner is a health content strategist focused on behavioural systems, clinical communication, and data-informed healthcare education.